Information for Families: Tongue-tie (Ankyloglossia)
- Details
- Created: Saturday, 12 November 2011 09:16
- Updated on Tuesday, 24 November 2015 15:21
Cite this article as:
Bowen, C. (2011). Information for Families: Tongue-tie (ankyloglossia) http://www.speech-language-therapy.com/ on [insert the date that you retrieved the file here].
The tongue
The most important articulator for speech production is undoubtedly the tongue. During speech, the amazing range of movements the tongue can make include tip-elevation, retraction, grooving, and protrusion.
Relatively short at birth, the tongue grows longer, and thinner at the tip, as we get older.
Functions of the tongue
As well as having a speech function, the tongue is needed for sucking, chewing, swallowing, eating, drinking, tooth and gum health, kissing, sweeping the mouth for food debris and other particles (such as hairs), warming the air during mouth-breathing, and oral play (for instance, poking the tongue out and waggling it about for fun).
Fraenum (fraenulum)
In anatomy, a fraenum (or fraenulum) is a small fold of tissue that checks or limits the movements of an organ part. Everyone has a lingual fraenum (lingual fraenulum) under the tongue. It is a thin, vertical fold of tissue with attachments to the under-surface of the tongue and to the floor of the mouth.
Ankyloglossia
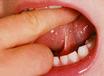
The terms 'ankyloglossia', 'short fraenum', 'short fraenulum', or 'tongue tie', refer to a restricted lingual fraenum due to a consolidation of tissue, usually leading to reduced mobility of the tongue.
It is commonly observed that a person with tongue-tie cannot protrude the tongue tip beyond the edges of the lower incisors, or to the maxillary alveolar ridge (behind the upper incisors). Sometimes when a person with tongue-tie attempts to protrude the tongue it forms a characteristic 'W' shape.
Will it stretch?
Parents of infants and toddlers with tongue-tie are sometimes advised that the tie will 'stretch', or 'break' permitting a free range of movement, as the child grows. These stretching and breaking phenomena have not been formally studied or documented in the medical or speech-language pathology literature.
Images of Tongue-tie
Dr Ghorayeb | Google Images | Carmen Fernando's Gallery
Potential effects of tongue-tie
1. Speech development
It is important to note that tongue-tie does not necessarily impair speech, in fact, it rarely appears to do so. Many individuals compensate well and have normal sounding speech, even those with the fraenum attached very close to the tongue tip. Some individuals with tongue-tie may have imprecise articulation, especially at speed.
"Most experienced speech-language pathologists would conclude that frenulectomy is rarely indicated for speech reasons unless it is very severe or there are concomitant oral-motor problems." Ann W. Kummer
2. Dental health
Cavities ('dental caries') can occur due to food debris not being removed by the tongue’s action of sweeping the teeth and spreading saliva.
3. Periodontic health
Gingivitis (gum disease) can develop, for the reason stated above.
4. Oral hygiene
Halitosis (bad breath) may be present, due to caries and accumulated food debris.
5. Eating and digestion
Some children with tongue-tie are messy eaters due to a restricted ability to tidy up inside and outside of their mouths while they are having a meal. Some are unable to circle their lips with their tongues in order to fully lick their lips. In extreme cases poor oral hygiene can lead to digestive complaints.
6. Sexual function
Restricted tongue movements may affect sexual expression.
7. Appearance
The tongue can be unduly obvious or unusual looking in some individuals, particularly when they are close up, or appear on video, film or TV.
8. Oral play
Children in particular may not be able to participate in play routines involving tongue movements and gestures.
9. Self esteem
It has been noted clinically that occasionally an older child or adult will be self-conscious, embarrassed or resentful about their tongue tie.
Examining for tongue tie
In a typical initial consultation the SLP/SLT conducts a case history interview and assessment, recording the following information:
- Identifying information (name, age, family details, etc)
- History including family history and language development
- Presentation
- Early feeding
- Feeding now
- Teeth
- Tongue Movements
- Appearance
- Oral Hygiene
- Saliva control (swallowing)
- Speech development history
- Speech assessment
Tongue tie surgery
Tongue-tie surgery (lingual frenectomy) involves more than just a simple clipping or a quick snip, but more involved tissue resection under general anaesthetic. It is therefore not recommended unless there is a good (speech, dental or other) justification for doing it.
Lingual frenotomy
Lingual frenectomy and lingual frenotomy are different procedures. Lingual frenotomy is often performed on newborns and neonates with tongue-tie to enable them to latch and suckle. Lingual frenotomy is sometimes referred to as "tongue clipping". It is done with a local anaesthetic.
Lingual frenectomy
The decision for toddler or child to proceed with frenectomy is arrived at through consultation between the client (if he or she is old enough), his or her parents, the SLP/SLT and the surgeon (and the family's GP in some instances).
Some parents/caregivers like to seek two SLP/SLT opinions to help them make their decision whether to not to proceed with tongue-tie surgery.
The potential for complications and discomfort need to be discussed by parents with the surgeon and anaesthetist.
Children should be assessed by a SLP/SLT prior to tongue tie surgery. Some require pre-operative exercises, and most require post-operative exercises under a SLPs/SLTs supervision.
Post-operative Exercises
The purpose of post-operative exercises
Post-operative exercises following tongue-tie surgery are not intended to increase muscle-strength or to improve speech, but to:
- Develop new muscle movements, particularly those involving tongue-tip elevation and protrusion, inside and outside of the mouth.
- Increase kinaesthetic awareness of the full range of movements the tongue and lips can perform. In this context, kinaesthetic awareness refers to knowing where a part of the mouth is, what it is doing, and what it feels like.
- Encourage tongue movements related to cleaning the oral cavity, including sweeping the insides of the cheeks, fronts and backs of the teeth, and licking right around both lips.
Will the exercises improve speech?
The exercises will not improve speech. If you want to improve speech, you have to work on speech.
The exercises must be individualised
Discuss these suggested exercises with YOUR child's speech-language pathologist / speech and language therapist before commencing them as they may not be suitable for your child. The SLP/SLP will modify them according to your child's age and requirements.
Encourage oral play
Encourage oral play generally, and do a selection of the following exercises, in any order, in 3 to 5 minute bursts, once or twice daily for 3 or 4 weeks post-operatively. Have a torch and hand-mirror handy. Make it fun.
Exercises
- Stretch your tongue up towards your nose, then down towards your chin. Repeat.
- You can vary the exercise above and make it more interesting by putting a dab of food in various positions above the top lip, to be retrieved with the tongue tip (You could call this game 'Elephant Tongue' and read books about elephants (e.g., 'Babar') to stimulate your child's interest in playing the 'tongue games' spontaneously at other times - not just when you are there.
- Open your mouth widely. Touch your big front teeth with your tongue with your mouth still open. Can you FEEL how tough your teeth are?
- Look in the mirror. Still with your mouth open wide, say dar-dar-dar, now say nar-nar-nar, now say tar-tar. Look in the mirror to see what your tongue is doing. Can you FEEL where it is?
- Lick your whole top lip from one side to the other.
- Now go back the other way.
- Lick your whole bottom lip from one side to the other.
- Go back the other way.
- See how many times you can lick your lips right around.
- Poke your tongue out as far as it will go.
- Shut your mouth and poke it into your left cheek to make a lump.
- Do the same on the other side.
- Now see if you can make your top lip fat without opening your mouth.
- Can you go in-out-in-out-in-out with your tongue? (demonstrate)
- Put your tongue behind your teeth and shut your mouth. Can you find your big top teeth with your tongue while your mouth is still shut? FEEL how tough your teeth are.
- Play your own version of copy cats, Simon Says or Follow the Leader incorporating the preceding movements.
Adolescents and adults with ankyloglossia
This article generates copious correspondence! Having read it, numerous young people and adults with tongue-tie write to ask if it is 'too late' for them to have a lingual frenectomy.
Since all speech-language pathology intervention is based on face-to face assessment it would be impossible, as well as unethical, for me to offer individual advice (see the site disclaimer). My suggestion to these correspondents is for them to start by seeking an opinion from a speech-language pathologist/speech and language therapist.
SLPs/SLTs as well as members of the community and medical practitioners vary in their views on the advisability of, and the necessity for, tongue-tie surgery for adults and children.
When frenectomy is performed, the operation is likely to be done by a general surgeon, an ENT surgeon, a cosmetic ('plastic') surgeon, or an oral surgeon.
The decision for an adolescent or adult to proceed with frenectomy is arrived at through consultation between the client, the SLP and, of course, the surgeon.
Many people report that they have found it difficult to access a surgical remedy when they ask for a referral from their own doctor, or approach a surgeon directly (without an SLP/SLT opinion).
Links
Ankyloglossia: To clip or not to clip? That's the question
An article by Ann W. Kummer writing in the ASHA Leader, 10 (17), 6-7, 30. (Dec 27, 2005).
Carmen Fernando (d. April 18, 2015): Tongue-tie: from confusion to clarity
'The purpose of this web site is to inform those with tongue tie, as well as their families and professional helpers, about the condition and how best to deal with it. This little-understood condition affects thousands of children and adults.'
Tongue-tie: Impact on Breast Feeding
This video, produced by a Canadian doctor, Evelyn Jain, MD, CCFP, IBCLC is intended to aid the physician in identifying tongue-tie and performing frenotomy. It demonstrates a comprehensive method of assessment of the impact of tongue-tie on breastfeeding, as well as a follow up management plan for the lactation consultant.

